Tendons are thick cords that join muscles to bones. Healthy tendon tissue mostly consists of mature type I collagen fibers which are normally organized into bundles of fibrils that run parallel along the length of the tendon. The longitudinal arrangement of the collagen fibers gives the tendon its tensile strength. The tensile strength in a tendon can be more than twice that of its associated muscle. As a result, tendons are rarely injured or torn.
There are also small amounts of type III collagen fibers present in healthy tissue. Type III collagen fibers are immature, thinner, unaligned with each other, and sometimes fail to link together to facilitate load- bearing.
Tendinosis
Tendinosis is chronic tendon degeneration that involves collagen deterioration. It can occur in any tendon throughout the body but usually occurs in the Achilles tendon, wrist tendon, elbow tendon, patellar tendon or rotator cuff. Tendinosis usually occurs at the boney attachment (where the tendon attaches to the bone), but can also occur in the middle of the tendon, most commonly seen in the Achilles tendon.
Type I Collagen Fibers:

Type II Collagen Fibers:
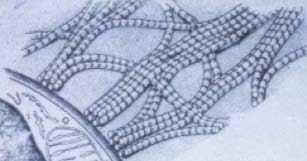
Symptoms include tendon pain when moved or palpated, stiffness and range of motion constraints as well as tendon thickening and lumps which can be Type II Collagen Fibers palpable or even visible in severe case. Clinically, tendon thickening is often present in older individuals who have had ongoing problems with tendinopathy, or in younger individuals who continually overload the tendon Tendinosis results when a tendon is continually overused from repetitive movements or strain without giving the tendon time to heal and rest. Even small movements such as clicking a mouse repeatedly can exert excessive tensile force on the tendon causing a reduction in the amount of type I collagen fibers and the proliferation of immature types III collagen fibers. These degenerative changes are triggered by the activation of a stress-activated protein kinase along with the initiation of programmed cell death. A microscopic view of tendinosis reveals an increase of immature type III collagen fibers, a loss of collagen continuity, an increase in ground substance (material between the body's cells), and a disorganized increase of non-productive vascularization.
Histopathologic analysis supports the hypothesis that tendinitis occurs secondarily to tendinosis, in other words, tendinosis precedes tendinitis. Since a healthy tendon is up to twice as strong as a muscle, a tendon is unlikely to tear before the muscle tears. If a tendon has already been degenerated at the cellular level, the tendon can become weaker than a muscle and will be injured before the muscle thus leading to tendinitis. Tendinosis is often responsible for the pain and burning in the affected area, decreased strength and flexibility, and aching during everyday activities. For patients who are elderly or with medical conditions such as diabetes, tendinosis is very common and can develop quickly.
Type II Collagen Fibers:

If tendon fiber tearing were the primary problem, the tissue would heal rather quickly. However, besides torn fibers; scar tissue, calcification, and very rarely, inflammatory cells are often found in conjunction with tendinosis. Not only is collagen rebuilding a slow process but healing tendinosis also requires many components including reversal of cellular damage, optimizing collagen production, improving tensile strength, and removal of scar tissue and calcification. Tendons do not receive the same amount of oxygen and blood that muscles do especially at the mid portion of the tendon and at the boney attachment where tendinosis occurs, thus making the healing of tendinosis difficult and lengthy. With current traditional treatment, an early stage tendinosis can take 6 to 10 weeks. However, if the condition is not taken care of promptly and becomes chronic, it can take 3 to 9 months based on severity.
Tendinitis
Tendinitis is a condition in which tendons become inflamed or irritated. Symptoms of tendinitis include tendon inflammation, acute pain, tenderness, and stiffness. Even though any tendon can develop tendinitis, it is most common in the shoulders, knees, elbows, heels, or wrists. These forms of tendinitis may also be called rotator cuff tendinitis, jumper's knee, tennis elbow, golfer's elbow, Achilles tendinitis, and carpal tunnel syndrome, respectively.
Tendinitis is usually caused by an acute injury resulting in micro-tears when a tendon which has undergone degenerative changes is overloaded with a tensile force that is too heavy and/or too sudden. The degenerated tendons lose their strength due to the loss of the parallel and aligned type I collagen fibers which are replaced by the bulky and weak type III collagen fibers, therefore, making it weaker and more vulnerable to injury.
In the event of the sudden tensile force overload on the degenerative tendon, the injury usually occurs at the musculotendinous junction where the muscle and tendon meet. Even in muscles where complete ruptures occur, such as the biceps brachii or triceps surae group, the rupture usually is at the musculotendinous junction.
Tendon Tear
Tendon tears usually occur due to trauma or when the tendon has degenerated and is more susceptible to an injury. In the event of a tendon injury, the tendon tears away from the bone or ruptures within the tendon itself. Rotator cuff tears occur frequently in overhead sports and in individuals who have a degenerated rotator cuff tendon. Untreated partial tears can progress to large rotator cuff tears. Achilles tendon tears also occur frequently from traumatic injuries when the tendon is subject to unusually high loads which can be due to a combination of chronic degeneration with exposure to high loads.
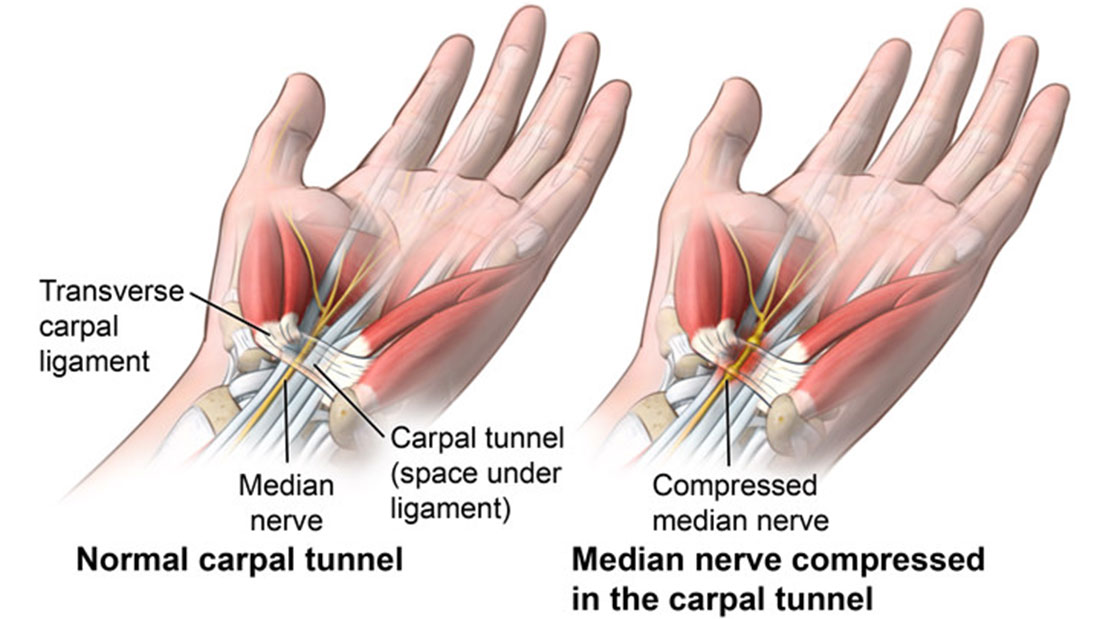
Carpal tunnel syndrome (CTS) is a condition that results from compression of the median nerve as it travels through the wrist and under the carpal tunnel. The tendons in the carpal tunnel become inflamed, compressing the median nerve and reducing control over the thumb and first three fingers. This can cause pain, numbness, tingling, and weakness in the hands, wrist, or forearm. Tendinosis in the forearm and wrist can cause a secondary carpal tunnel syndrome because the thickening of the tendons along with excess ground substance and swelling of the surrounding tissue can crowd and compresses the median nerve. According to an estimate done by the U.S Centers for Disease Control and Prevention, 3.1% of employed adults between 18 and 64 had carpal syndrome in the past year.