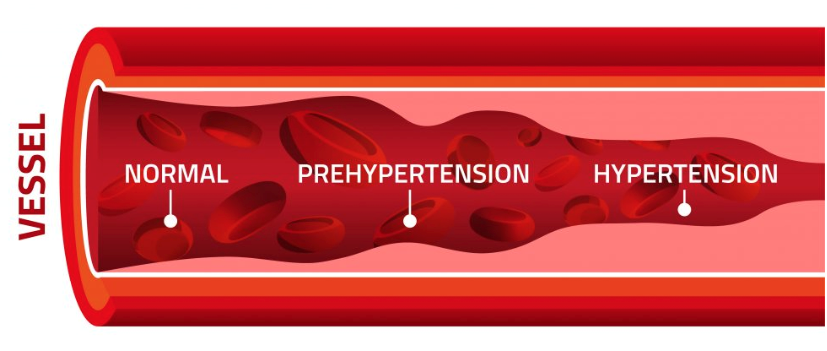
Blood pressure is a measurement of the force against the artery walls as the heart pumps blood through the body. High blood pressure (hypertension) is a condition in which the long-term force of the blood against the artery walls is consistently too high. If high blood pressure is left uncontrolled, it can cause severe damage to many organs including the heart, kidneys, brain, and blood vessels.
A blood pressure reading, given in millimeters of mercury (mm Hg), contains two numbers. The first number measures the pressure in the arteries when the heart beats (systolic pressure). The second number measures the pressure in the arteries between beats (diastolic pressure).
Blood pressure measurements fall into four categories:
- Normal blood pressure: below 120/80 mm Hg
- Elevated blood pressure: systolic pressure ranging from 120 to 129 mm Hg and a diastolic pressure below 80 mm Hg
- Stage 1 hypertension: systolic pressure ranging from 130 to 139 mm HG or a diastolic pressure ranging from 80 to 89 m HG
- Stage 2 hypertension: systolic pressure of 140 mm Hg or higher or a diastolic pressure of 90 mm Hg or higher.
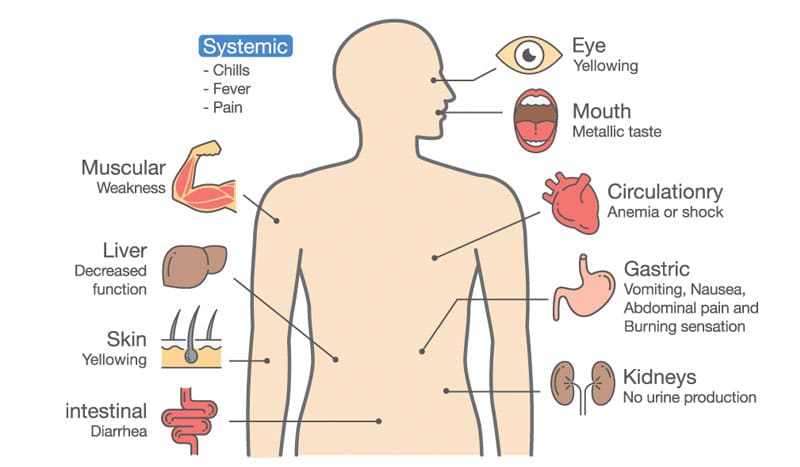
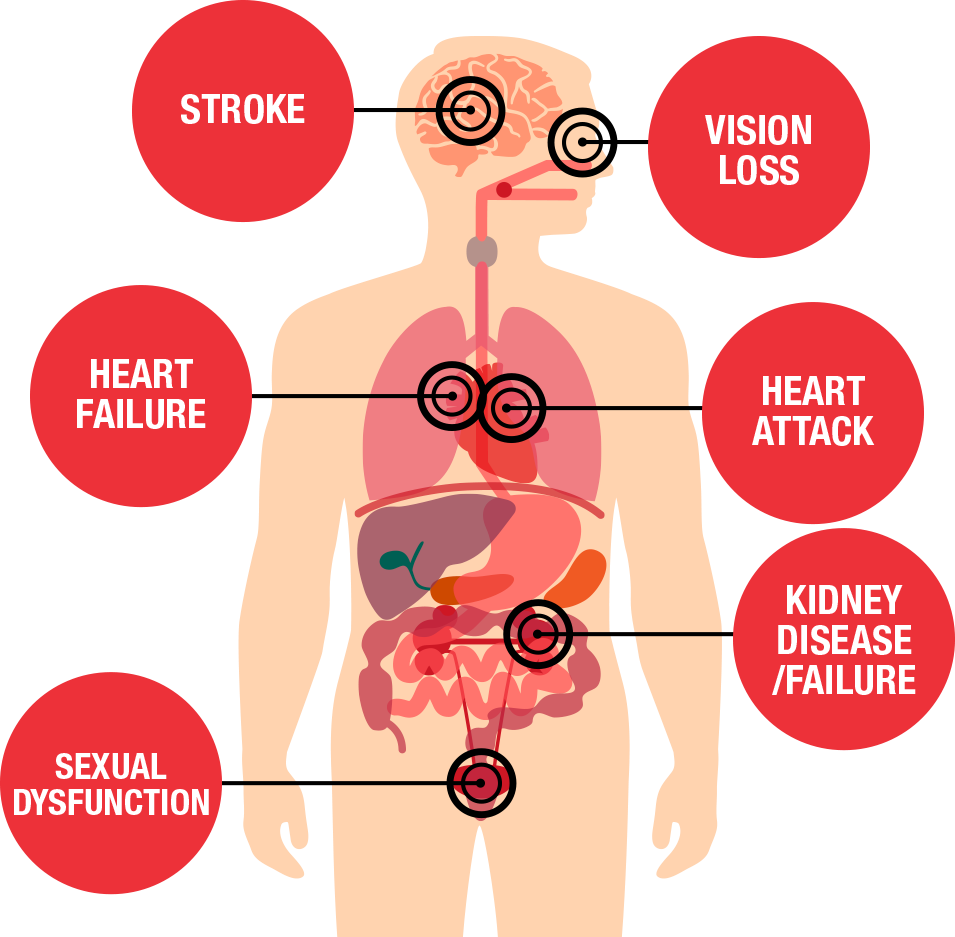
Most patients do not experience any symptoms, even if their blood pressure is dangerously high. This is why the condition can be referred to as "the silent killer." Few may experience headaches and shortness of breath, but these typically don't appear until high blood pressure has reached a life-threatening stage. Although there may not be prominent symptoms, high blood pressure can cause serious complications. The excessive pressure on the artery walls can damage the blood vessels as well as the organs. This can lead to complications including stroke, heart attack, aneurysm, heart failure, weakened blood vessel in the kidneys which may result in chronic kidney disease or kidney failure, metabolic syndrome, sexual dysfunction, vision loss, and memory loss.
Blood pressure is regulated through the renin-angiotensin system (RAS), or renin-angiotensin-aldosterone system (RAAS) which is a hormone system that regulates blood pressure, fluid and electrolyte balance, as well as systemic vascular resistance. The liver and kidneys play a vital role in regulating blood pressure using a hormone system.
The RAS regulates blood pressure by modulating vascular smooth muscle contractions. When blood pressure is reduced, the blood flow to the kidneys is also reduced. The reduced blood flow to the kidneys triggers the juxtaglomerular cells in the kidneys to convert pro-renin in the blood to renin which is secreted directly into circulation. Renin will catalyze the formation of angiotensin I from angiotensinogen which is synthesized by the liver. Angiotensin I is subsequently converted to angiotensin II by the angiotensin-converting enzyme (ACE) found in the lungs. The angiotensin II then binds to the receptors on the blood vessel cells. The type I angiotensin II receptor (AT1) will be become activated upon binding to angiotensin II and trigger activation of G-proteins and protein kinase to initiate the signal transduction inducing vascular smooth muscle contractions to raise blood pressure. Over activation of RAS can cause high blood pressure.
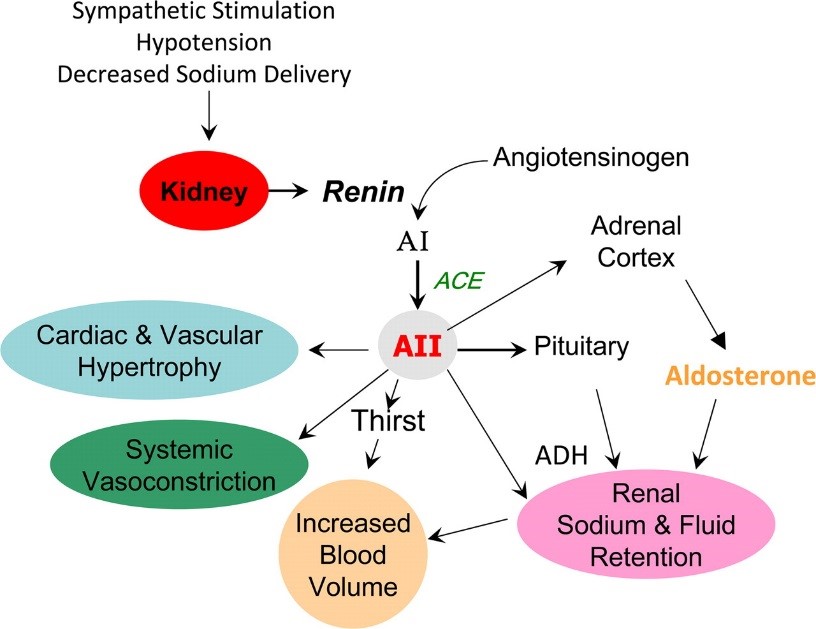
The RAAS regulates blood pressure by modulating the kidney's mineral absorption function. The angiotensin II also stimulates the secretion of aldosterone from the adrenal gland to increase the reabsorption of sodium and water into the blood by the kidneys, while at the same time excreting potassium, to maintain electrolyte balance. This increases the volume of extracellular fluid in the body as well as the blood pressure. Overactivation of RAAS can cause high blood pressure.
There are two types of high blood pressure. The first is called primary hypertension that tends to develop gradually over time. The second is referred to as secondary hypertension and tends to appear suddenly. Various conditions and medications can lead to secondary hypertension.
Many liver conditions can affect blood pressure due to their overactivation of RAS and RAAS. Fatty liver disease and diabetes stimulate the hepatic expression of RAS components such as ACE and angiotensin receptors. The increased levels of renin, ACE, and angiotensin receptor levels and increased sensitivity of AT1 signal transduction pathway to angiotensin II and cause over activated RAS and RAAS resulting in the development of high blood pressure.
High blood pressure may also be caused by vascular hypersensitivity due to hyperactive Angiotensin II Receptors transduction pathway. The stimulants such as renin, ACE or angiotensin II might be normal. However, the vascular system will overly respond to the stimulants with increased levels of vasocontraction due to over response of AT1 signal transduction pathway. Patients with liver conditions often also have vascular hypersensitivity.
Atherosclerosis is a condition involving the narrowing of the blood vessels due to the build-up of fats, cholesterol, and other substances on the artery walls. Atherosclerosis usually develops from the lower part of the body and progress upward. The narrowed renal arteries can lead to declined kidney function and/or structure. The resulting reduced blood flow to the kidneys causes an excess amount of renin production, which raises blood pressure. Patients usually develop renal atherosclerosis, nephrosclerosis, with high blood pressure before having heart atherosclerosis. The time frame is usually 5 years.
Chronic kidney disease can also cause reduced blood flow to the kidneys resulting in overproduction of renin and aldosterone. More importantly, the poor kidney function can also cause retention of water and salt leading to high blood pressure.